The Electronic Prescribing (eRx) Incentive Program was created by Section 132 of the Medicare Improvements for Patients and Providers Act of 2008 (MIPPA). As of January 2009, this act authorized a separate incentive program for electronic prescribers—separate from and in addition to the Physician Quality Reporting System (PQRS, formerly PQRI).
Providers do not have to participate in PQRS to participate in eRx. The eRx program is still voluntary and providers do not have to register unless participating in the group reporting option.
What is eRx?
Electronic prescribing is the transmission of prescriptions or prescription-related information through electronic media. The eRx program applies to both medication prescriptions and durable medical equipment (DME) that requires a prescription. However, eRx does not apply to spectacle prescriptions or contact lens prescriptions.
Electronic prescribing occurs between a prescriber, dispenser, pharmacy benefit manager or health plan, and can take place directly or more commonly through an intermediary (e.g., eRx network).
Why eRx?
There are a number of reasons for the push toward e-prescribing, including safety and patient convenience.
• Safety. E-prescribing reduces the risk of medication errors. To start, handwriting issues and errors are eliminated. Second, the systems provide real-time checks for dangerous drug allergies by displaying all the information a pharmacy has about the individual’s allergies as well as other medications he or she is taking at the time you are prescribing.
Third, eRx reduces the potential for fraud or tampering by patients and eliminates the potential to alter an Rx (e.g., increase number of pills or refills), which is especially important for controlled substances. (Note: Controlled substances can now be eRx per the DEA.)
Finally, providers have access to a patient’s medication history from different sources at the time they are prescribing medication. This allows providers a more informed check for potentially harmful drug interactions.
 • Patient convenience. By sending a prescription directly from your computer to a pharmacy, the Rx arrives at the pharmacy before your patient even leaves your office. This saves the patient time in the prescription drop off and pick up process. By eliminating the paper Rx, the patient cannot lose the prescription; this saves your staff time and energy that would be spent recreating that prescription. And time, we know, equals money.
• Patient convenience. By sending a prescription directly from your computer to a pharmacy, the Rx arrives at the pharmacy before your patient even leaves your office. This saves the patient time in the prescription drop off and pick up process. By eliminating the paper Rx, the patient cannot lose the prescription; this saves your staff time and energy that would be spent recreating that prescription. And time, we know, equals money.
• Practitioner convenience. The eRx program was designed to give practitioners access to patient eligibility and formulary information, which they can use to better determine the most clinically appropriate and cost effective medication. With eRx, you do not have to deal with those pesky phones calls from the pharmacy to ask you to substitute another medication. Also, keep in mind that because the entire prescribing process is automated, new prescriptions and renewal requests come directly into your e-prescribing application for authorization—saving you time and staff resources.
Finally, as an added bonus, electronic Medicaid prescriptions can be filed online. Since 2008, all written Medicaid prescriptions must be on a tamper-resistant prescription pads. But, with eRx, prescribing practitioners do not have to purchase the expensive tamper-resistance pads. As of January 1, 2012, practitioners will not be able to send Medicare Part D prescriptions by fax—they will only be accepted if handwritten or submitted via eRx.
What is an Qualified eRx System?
A qualified eRx system must be able to do all of the following:
1. Generate a complete medication list that incorporates data from pharmacies and benefit managers, as available.
2. Select medications, transmit prescriptions electronically using the applicable standards and warn the prescriber of possible undesirable or unsafe situations.
3. Provide information on lower-cost, therapeutically appropriate alternatives. (Tiered formulary information, if available, meets this requirement.)
4. Provide information on formulary or tiered formulary medications, patient eligibility and authorization requirements received electronically from the patient’s drug plan.
It is important to understand that e-prescribing software and EHR systems that transmit prescriptions to pharmacies only by fax are not considered to be “qualified systems” under this program.
 How to Get Started on eRx?
How to Get Started on eRx?
GetRxConnected, created by The Center for Improving Medication Management, is a site that provides a step-by-step process to help transition from paper-based prescribing to e-prescribing with clinical decision support and pharmacy connectivity (see “Steps to Get Connected”).1 More than 75% of the nation’s pharmacies process prescriptions electronically, so most regions will have pharmacies that are in the “electronic network.”2,3
GetRxConnected helps prescribers and practice management professionals assess the financial impact of e-prescribing with an interactive feature to calculate an estimated value of the time and resources their practices are currently dedicating to the manual processing of prescriptions.
What is the Cost for eRx?
The GetRxConnected program will walk you through the necessary steps to get started and the cost analysis for your individual practice. The cost per year of an eRx system can range from free to $800.1
Overview: 2011 eRx Bonus Program
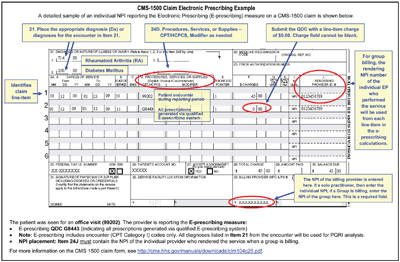
An example of a 2009 eRx claim form.
The 2011 eRx Bonus Program works in much the same way as PQRS. The provider will use the code (numerator) of G8553—at least one prescription created during the encounter was generated and transmitted electronically using a qualified eRx system. This code is added to the Medicare claim for the services provided at the time the prescription was issued. It is added as a line item on the claim—like the evaluation and management visit codes—but the price is listed as $0.00 (or a very small amount like $0.01, if your billing system does not allow zero dollar amounts).
The 2011 Incentive Payment for eRx will be 1% of all your Medicare claims for 2011. However, this bonus is not available to professionals who receive the 2011 Medicare EHR Incentive payment because eRx is an integral part of the EHR incentive program. The reporting period runs from January 1 through December 31, 2011. Keep in mind that, although we are well into 2011, there is still time to qualify for this bonus; the requirement is for an individual to report at least 25 unique eRx events during the entire reporting period.
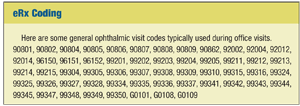
There are some other reporting mechanisms that use qualified registry and/or group reporting in addition to claims-based reporting. The G8553 code can be used for any Medicare patient visit for which one (or more) of the applicable visit codes is used (see “eRx Coding”).
For claims-based reporting (paper or electronic filing), the G8553 must be reported on the claim(s) with the billing code(s) that represent the eligible encounter for the same beneficiary, for the same date of service (DOS), by the same eligible professional who performed covered service as payment codes (i.e., same individual National Provider Identification (NPI) number).
When a group bills, the individual rendering/performing physician’s NPI must be placed on each line item, including all allowed charges and quality-data line items. Solo practitioners should follow their normal billing practice of placing their individual NPI in the billing provider field (#33a on the CMS-1500 form or the electronic equivalent). While not a requirement for solo practitioners, adding the provider NPI number on each line item is always a good practice.
As with PQRS, eRx claims may not be resubmitted for the sole purpose of adding or correcting an eRx code. Phone requests for prescription refills do not count; no visit means no claim. All claims must be submitted before February 24, 2012 to be included in the analysis. Therefore, remember to promptly file all claims for services furnished toward the end of the reporting period. Please remember that claims that are resubmitted only to add quality data codes (QDCs) will not be included in the analysis.
On the Explanation of Benefits (EOB) you received back from the claim, the eRx G-code line is denied (but tracked) and sent to the National Claims History (NCH) database. Remittance Advice (RA) includes a standard denial remark code N365 with the statement, “This procedure code is not payable. It is for reporting/information purposes only.” However, the N365 code does not indicate whether the eRx G-code is accurate for that claim; it only indicates that the eRx G-code passed into NCH.
Addtional eRx Reporting Mechanisms
While registry reporting does exist there is currently no registry appropriate for optometry. There are two phases for Group Reporting. For Group Reporting I, a practice must have 200 or more providers. For Group Reporting II, a practice must have between two and 199 providers.
In order to qualify for one of the two groups for Group Reporting, a group must have completed the nomination process and been accepted by the Centers for Medicare and Medicaid Services (CMS). This is a complicated process. If a group practice in interested in this type of reporting for 2012, you can find more information at CMS.2
Penalties for Not Successfully Using eRx
In 2012, you will get a 1% reduction if you do not use eRx in 2011 but report at least 10 eRx events prior to June 30, 2011. However, CMS reports that optometrists will not be penalized 1% for 2012 if they did not meet this requirement.4 Optometrists will likely be penalized in future years; however, for 2012, the exemption stems from the wording of the definition in the final rule: “The eligible professional is a physician (M.D., D.O. or podiatrist), nurse practitioner or physician assistant as of June 30, 2011.” No adequate explanation was found for the omission of optometry even though, under CMS, optometrist is defined as a physician.
Per CMS, providers must report eRx measure 25 times over 12 months in 2011 to avoid the 2013 penalty.
The eRx bonus structure is:
• 2011 and 2012: 1.0% of allowed charges.
• 2013: 0.5% of allowed charges.
The eRx penalty structure is:
• 2012: Not successful e-prescribers in 2011 without hardship exception: 1.0% payment reduction allowed charges (optometry exempted).
• 2013: Not successful e-prescribers in 2011 without hardship exception: 1.5% payment reduction allowed charges (optometry is not expected to be exempted, so begin eRX now).
• 2014: Not successful e-prescribers in 2013 without hardship exception: 2.0% payment reduction allowed charges.
A Last Bit of Advice
Optometrists should begin eRx as soon as possible to qualify for the 2011 1% bonus and avoid penalties in future. Remember to visit GetRxConnected for the tools to get started in eRx.1 Remember that you cannot receive the 2011 eRx bonus payment if you qualify for and receive the 2011 EHR incentive payments.
Electronic prescribing is definitely a paradigm shift. But once you eRx, you will not go back to those little paper pads. The patients are delighted and your life is easier. And, more money from Medicare is not too shabby either.
Rebecca Wartman, O.D., is in private practice in Asheville, N.C., and is a past president of the North Carolina State Optometric Society (NCSOS). Dr. Wartman currently chairs the NCSOS Third Party Committee.
1. GetRXConnected. Electronic Prescribing Readiness Assessment. 2011. Available at:
www.getrxconnected.com/OPTOMETRIC/site.aspx (accessed August 2011).
2. LearningAboutEPrescriptions. What is an E-Prescription? Surescripts Network. Available at:
www.learnabouteprescriptions.com/what-is-eprescription.aspx (accessed August 2011).
Surescripts Network. Advancing Healthcare in America. 2009-2010. Available at:
www.surescripts.com/media/515306/2009_national-progress-report.pdf (accessed August 2011).
Centers for Medicare and Medicaid Services. E-Prescribing Measure. 2011 Jul. Available at:
www.cms.gov/ERxIncentive/06_E-Prescribing_Measure.asp (accessed August 2011).


