Is there a perfect fit? For a keratoconic, the fit of a contact lens could always be tweaked just a little bit. The question, however, is deciding which health and/or vision factors would make this a beneficial and worthwhile change. Any design changes made to affect the gas-permeable (GP) fitting relationship should be significant in nature. For a fitting tip checklist, visit www.gpli.info.
Patients that present with keratoconus almost always have a list of problems and visual concerns. In this article, we will troubleshoot the most common complications with keratoconus that present with GP lenses.
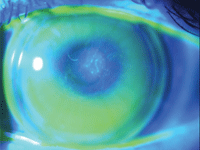
1. Apical bearing and subsequent swirl staining.
Corneal Abrasions and Erosions
A common issue that our patients face is recurrent corneal abrasions and/or chronic epithelial erosions. The classic histopathology in keratoconus includes iron deposition in the epithelium, thinning of the stromal layer and breaks in Bowman’s layer. The average epithelial thickness is approximately 52µm.1 The epithelium over the cone in corneas with keratoconus can be much thinner, around 25µm, and this can be surrounded by epithelial thickening to compensate for stromal thinning and steepening.2
Recurrent abrasions and epithelial breaks start with the pathogenesis of keratoconus, but will be exacerbated by contact lens wear. Low levels of the protein -enolase in the epithelial cells in keratoconus affect cell migration during wound closure and therefore, a loss of interactions with the proteins of the cell matrix.3 This will lead to disassembly of that matrix and might result in corneal thinning.
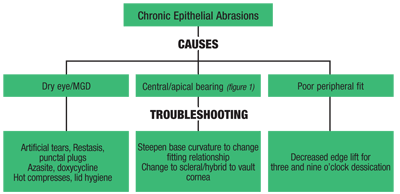
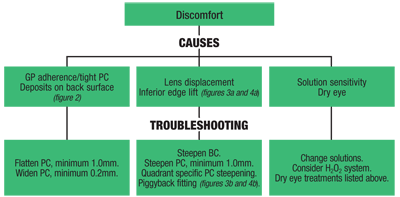
An additional theory is that epithelial trauma and persistent damage can produce inflammatory cytokines, which result in stromal thinning from keratocyte apoptosis (see “Chronic Epithelial Abrasions” p 30).4 Although chronic epithelial issues will lead to discomfort, there are other causes that may prohibit day in and day out comfort, leading to a limited wear schedule (see “Discomfort,” below).
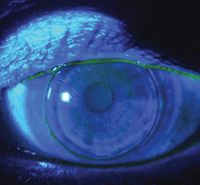
2. This patient needs a flatter and wider peripheral curve.
Glare and Halo
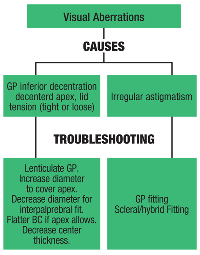
Another major challenge is visual aberrations including glare, ghosting or multiple images, and halos (see “Visual Aberrations” p 31). There are some patients who seem to have comfort or lens stabilization issues, regardless of what GP lens style or design you select. Patients who tend to get recurrent abrasions from the mechanical bearing of the lens on the apex of their cone are always losing lenses or finding them painfully displaced on the eye, which presents additional challenges.
One option is piggybacking (soft lens placed under the hard lens), a technique that does not always solve the problem and counterproductively, may even cause additional concerns stemming from multiple hands touching the lens.
An Alternative to Consider
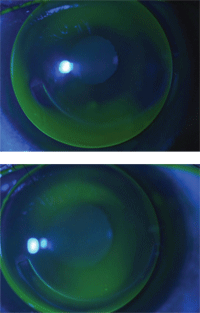
3a. Inferior edge lift in a
keratoconus patient post-Intacs. 3b. Asymmetric corneal technology
applied to inferior 6 o’clock edge lift with improved fit.
A great alternative for our patients may be hybrid lenses, which would allow for greater stability and often times increased comfort. Although it can be costly, ClearKone (SynergEyes) is one particular lens that seems to work well for keratoconus. Similar to scleral lenses, this particular hybrid lens is great at relieving the mechanical pressure the average GP contact lens places on the apex of a cone by vaulting entirely over the cornea. In fact, it is generally able to clear most keratoconic cones.
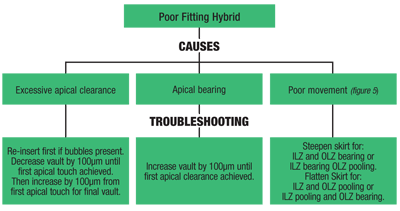
The design is such that the soft skirt—RGP junction—is inside the limbus with the skirt extending on the sclera at a typical soft lens diameter of 14.5mm. The junction is defined by two areas: the outer landing zone (the region of the soft lens) and the inner landing zone (the RGP lens portion).5 Unlike standard GP fitting practice, these lenses are fit not by base curvature, but rather vault—which describes the relative depth of the lens. The parameter that can be altered is the soft skirt curvature, which comes in flat, medium and steep options (see “Poor Fitting Hybrid,” below).
Even with this straightforward approach, it is not always possible to avoid fitting problems. One of the most common obstacles with these lenses is the development of a tight fitting lens which can cause corneal edema, pain, and difficulty removing the lens. There are also cases of such advanced keratoconus that there simply isn’t a hybrid lens manufactured which can adequately clear the corneal apex. In failed hybrid cases such as these, scleral lenses may be an excellent alternative. Greater availability of parameter ranges allow for more flexible fitting options. And, larger diameters (15mm to 18mm) tend to result in increased comfort due to less lid interaction.
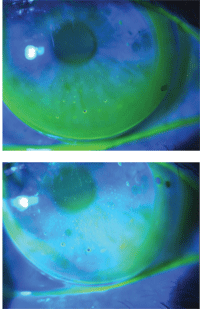
4a. Inferior edge lift with dimple veiling. 4b. Quadrant specific edge lift inferiorly with the further steepening of mid-peripheral fit. Another option is to make the lens smaller.
If, despite best efforts, the patient fails with rigid lenses of any modality in the eye, whether to due fitting issues or simply intolerance, there is a new wave of soft lenses specifically for the use of keratoconus. Soft K (Acculens) and KeraSoft IC (UltraVision) are examples of two such keratoconus soft lenses recently on the market. These lenses are designed with a thick optic zone to create structural stability for improved vision, yet maintain the comfort of soft lenses. Time will tell how these lenses perform in the world of keratoconic lenses.
GP contact lenses offer good vision for those with keratoconus and irregular corneas. Troubleshooting your patient’s contact lens and visual problems by providing GP lens changes or alternatives such as piggybacking, hybrid lenses, scleral lenses and custom soft lenses will help them achieve good, comfortable vision. And, they will thank for all your patience and effort.
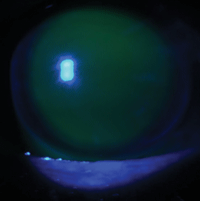
5. Excessive central pooling is seen with OLZ bearing and ILZ pooling. Two changes to improve this fit: reduce the vault by 100 µm or flatten the skirt curvature.
Dr. Hill Vanderhoof graduated from University of Missouri College of Optometry and completed a residency in ocular and refractive surgery. fellow in the American Academy of Optometry, she has transitioned to primary care in Denver, Colo. but still specializes in complicated contact lens fittings.
Dr. Sztipanovits graduated from UC Berkeley School of Optometry and completed a residency in ocular and refractive surgery. A diplomate of the American Board of Optometry, she is an instructor in ophthalmology and visual Sciences at Vanderbilt University, specializing in complicated contact lens fittings.
1. Wang M. Keratoconus and Keratoectasia. Thorofare, NJ: Slack Incorporated, 2010.
2. Reinstein DZ, Archer TJ, Gobbe M. Corneal epithelial thickness profile in the diagnosis of keratoconus. J Refract Surg. 2009 Jul;25(7):604-10.
3. Srivastava OP, Chandrasekaran D, Pfister R. Molecular changes in selected epithelial proteins in human keratoconus compared to normal corneas. Mol Vis. 2006 Dec 20;12:1615-25.
4. Hwang JS, Lee JH, Wee WR, Kim MK. Effects of multicurve RGP contact lens use on topographic changes in keratoconus. Korean J Ophthalmol. 2010 Aug;24(4):201-6.
5. SynergEyes. ClearKone Fitting Information. 2010 Sep. Available at:
www.synergeyes.com/ClearKoneContent.htm (accessed March 2012).


