Eye care professionals often mistakenly believe that a multifocal contact lens trial can indicate whether a cataract patient is a good candidate for a multifocal intraocular lens. For many reasons, this is simply not true. For example, if a patient has a cataract, their vision is going to be blurred no matter how well the contact lens is fit. Also, elderly patients are more likely to have ocular surface disease, which can cause fluctuations in vision with multifocal contact lens use.1,2 This also occurs with IOLs, but to a lesser extent.
Keep in mind that multifocal IOLs have different optics than the multifocal contact lenses we have available today. Also, multifocal contact lens wearers can be plagued by other fitting problems. Multifocal contact lenses, for example, can decenter and flex while on the eye affecting visual acuity.
In this article, I will outline the various multifocal IOL options and how to pick the right candidate for implantation.
The Multifocal IOL Market
There are currently three multifocal IOLs available in the United States, and each has a different design.

The Tecnis Multifocal has a full-diffractive posterior surface, which makes the
diffractive optics pupil independent.
• ReStor. The ReStor IOL (Alcon) uses an apodized diffractive design on the front surface. It is a single piece, aspheric lens that comes in two add powers. The 4.0 version gives a +3.20D add power in the spectacle plane, while the 3.0 version gives a +2.50D add at the spectacle plane.
This lens works well with patients who require a stronger reading add and have a pupil that still constricts with light and accommodation.
• Tecnis. The Tecnis (Abbott Medical Optics) IOL uses a full-aperture diffractive design on the posterior surface that splits light and distributes it among the near and distance foci.
The full-aperture diffractive design works well with patients who have a larger pupil size and who do near work in a dimmer lighting environment. The anterior surface has an aspheric design to compensate for the spherical aberration of the cornea to improve night vision
• ReZoom. The ReZoom (Abbott Medical Optics) IOL uses concentric refractive zones to produce near and distance images. The ReZoom IOL is most similar to today’s multifocal contact lenses that have concentric rings of power. However, the ReZoom lens is used less frequently then the diffractive IOL because of increased nighttime visual side effects such as halos around headlights.3,4
One could argue that fitting a multifocal contact lens is a good psychological indicator for the success of clear lens exchange surgery. Although today’s multifocal contact lenses provide good vision, they still compromise the distance and night vision to a small degree. If a patient found this compromise intolerable, it may be an indication that they are going to have a tough time with the multifocal IOL.
Ideally, we would be able to do a test to determine if a patient is going to adapt to a multifocal IOL before they have surgery. Unfortunately, there is currently no preoperative test that demonstrates what the vision would be like with a diffractive IOL.
If a patient is concerned about the compromised night vision with a multifocal IOL, but would still like less dependence on reading glasses, you can try implanting an accommodating IOL such as Crystalens (Bausch + Lomb). I find that while accommodative IOLs give better night vision, multifocal IOLs offer better near vision. The Synchrony IOL (Abbott Medical Optics), an accommodating IOL that may have stronger near results, is currently awaiting FDA approval.
Selecting the Right Candidate
How do we determine who is a good candidate for multifocal IOLs? Eye care practitioners agree that the key is to carefully select your patients and to take the time to educate them about outcomes and side effects before surgery.

The ReStor IOL must be centered well to give the best image quality.
A good candidate for multifocal IOLs is someone who has an easy-going, laid back personality, is not particular about their vision and is motivated to see at near without glasses. In contrast, a poor candidate is someone who is never satisfied with his or her vision correction, is overly demanding and/or frequently drives at night. I recommend taking extra care with patients who are obsessive-compulsive and/or have high astigmatism. There is also a reported case of a patient with Meniere’s disease who experienced problems adapting to a multifocal IOL.5
Astigmatism is not an absolute contraindication, since it can be treated with limbal relaxing incisions (LRI) or corneal refractive surgery. I prefer corneal refractive surgery over LRIs at my office because of its greater predictability.6,7 A toric design for ReStor multifocal IOL is currently available internationally but has not been FDA approved in the United States at this time.
A patient’s perception of a good visual result depends largely on their preoperative condition. For example, a 70-year-old +4.00 hyperope who has dense cataracts will be thrilled with the results of multifocal IOL implantation. However, a 55-year-old -2.00 myope with mild nuclear sclerosis is going to be a lot more particular about the end result of the surgery.
Patients should be educated about what to expect from their vision after surgery. We tell patients they will have glare and halo immediately following the procedure, but it will get better with time.
The vision with multifocal IOLs requires some neuroadaptation. It may take six to 12 months before the brain fully adapts to the multifocal image the eye receives with a diffractive IOL. This may be why patients with peripheral vestibular disorders, such as Meniere’s disease, do not do well with multifocal IOL implantation. Retinocortical processing of visual information is impaired in these patients, which may make it more difficult for them to adapt.5
If the patient is unable to adapt to the optics of a multifocal IOL, and no other treatments can improve the vision, your patient may require an explantation of the lens.
One final word of advice: Do not over-promise the quality of near vision post-operatively. Although near vision is generally adequate for the majority of patients, some must still wear reading glasses in certain situations.
Addressing the Dissatisfied Patient
Most patients report that they are happy with their vision in multifocal IOLs.8-11 However, some patients do express dissatisfaction and require further treatment to relieve their symptoms.12-15
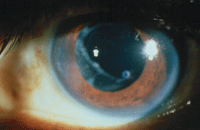
Capsular fibrosis can decrease vision after surgery and easily can be treated with a YAG capsulotomy procedure. (Photo: Tammy Than, O.D.)
A recent study evaluated symptoms, etiology of complaints and treatments for 76 eyes of 47 patients dissatisfied with their surgery.12 In this study, 69 eyes (90.8%) were treated with the 4.0 ReStor IOL, four eyes (5.3%) were fitted the 3.0 ReStor IOL, two eyes (2.6%) with the Tecnis IOL and one eye (1.3%) with the ReZoom IOL.
Of the 76 eyes, 94.7% (72 eyes) reported unsatisfatory vision and 38.2% (29 eyes) reported dysphotopsia. Patients were treated with refractive surgery, glasses, miotic eye drops, capsulotomy and other surgical procedures. Of the patients who reported problems, only 4% were unable to have their problem resolved and requested explantation of the IOL.12
If your patient experiences blurred vision from a residual refractive error, I recommend part-time spectacle wear or corneal refractive surgery. We find that patients experience good results with LASIK or PRK surgery after cataract surgery.
Elderly patients and patients with epithelial basement membrane dystrophy (EBMD) are at higher risk for developing loose epithelium during flap creation.16 For that reason, we often recommend PRK surgery instead of LASIK for our post-cataract patients.
Doctors are quicker to treat posterior capsular opacification in a multifocal IOL patient than in those with a monofocal IOL.17,18 Posterior capsular opacification increases unwanted symptoms of blurred vision and increased glare and halos after surgery.
It is important to make sure the patient understands that, once the posterior capsulotomy procedure is performed, we typically do not recommend lens explantation. If a patient reports that he did well with the lens at first and later experienced blurred vision, I know it is from capsular opacification, assuming no new ocular anomaly is present. However, if the patient has never been happy, I discuss the option of lens explantation before we perform a capsulotomy. Once the capsulotomy has been performed, the risk of surgical complications with explantation increases.
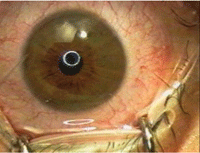
PRK surgery can be done over the
multifocal IOL to correct any residual
refractive error.
Even though nighttime vision problems can be caused by the optics of the multifocal IOL, other causes should be ruled out. A decentered IOL can increase glare and halos.19 It has been shown that as little as 0.3mm decentration of the multifocal IOL can cause symptoms.19
There are a number of pre-operative selection criteria that should be used in determining if a patient is a good candidate for multifocal IOL, an accommodating IOL or a monofocal IOL. The doctor should consider the patient’s distance and near visual needs, occupation, history (including any previous refractive surgery), pupil size in dim and bright light, and the overall ocular health. These pre-operative factors will guide the doctor in his recommendation of what type of IOL should be recommended.
There is no diagnostic test that determines who is a good candidate for multifocal IOLs at this time. However, you can still have success by choosing the right candidates for surgery, reviewing all the information regarding the lenses prior to surgery and referring back to your surgeon for any enhancements that may improve their vision.

Dr. Polk is the clinical director of TLC Laser Eye Center in St. Louis and an adjunct assistant professor at University of Missouri, St. Louis College of Optometry.
1. Guillon M, Maissa C. Tear film evaporation—effect of age and gender. Cont Lens Anterior Eye. 2010 Aug;33(4):171-5.
2. McGill JI, Liakos GM, Goulding N, Seal DV. Normal tear protein profiles and age-related changes. Br J Ophthalmol.1984 May;68(5):316-20.
3. Choi J, Schwiegerling J. Optical performance measurement and night driving simulation of ReSTOR, ReZoom, and Tecnis multifocal intraocular lenses in a model eye. J Refract Surg. 2008 Mar;24(3):218-22.
4. Chang DF. Prospective functional and clinical comparison of bilateral ReZoom and ReSTOR intraocular lenses in patients 70 years or younger. J Cataract Refract Surg. 2008 Jun;34(6):934-41.
5. Gatzioufas Z, Osvald A, Schroeder AC, et al. A serious refractive multifocal intraocular lens complication in Meniere’s Disease. Optom Vis Sci. 2010;87(6):448-9.
6. Roman S, Auclin F, Baudouin C. Limbal relaxation incisions to correct preexisting astigmatism during cataract surgery. J Fr Ophthalmol. 2009 Jun;32(6):390-5.
7. Mendicute J, Irigoyen C, Ruiz M, et al. Toric intraocular lens vs. opposite clear corneal incisions to correct astigmatism in eyes having cataract surgery. J Cataract Refract Surg. 2009 Mar;35(3):451-8.
8. Mester U, Hunold W, Wesendahl T, et al. Functional outcomes after implantation of Tecnis ZM900 and Array SA40 multifocal intraocular lenses. J Cataract Refract Surg. 2007 Jun;33(6):1033-40.
9. Packer M, Chu YR, Waltz KL, et al. Evaluation of the aspheric Tecnis multifocal intraocular lens: one-year results from the first cohort of the food and drug administration clinical trial. Am J Ophthalmol. 2010 Apr;149(4):577-84.
10. Goes FJ. Visual results following implantation of a refractive multifocal IOL in one eye and a diffractive multifocal IOL in the contralateral eye. J Refract Surg. 2008 Mar;24(3):300-5.
11. Javitt JC, Steinert RF. Cataract extraction with multifocal intraocular lens implantation: a multinational clinical trial evaluating clinical, functional, and quality-of-life outcomes. Ophthalmology. 2000 Nov;107(11):2040-8.
12. De Vries NE, Webers Ca, Touwslager WR, Bauer NJ. Dissatisfaction after implantation of multifocal intraocular lenses. J Cataract Refract Surg. 2011 May;37(5):859-65.
13. Muftooglu O, Prasher P, Chu C, et al. Laser in situ keratomileusis for residual refractive errors after apodized diffractive multifocal intraocular lens implantation. J Cataract Refract Surg. 2009 Jun;35(6):1063-71.
14. Jendritza BB, Knorz MC, Morton S. Wavefront-guided excimer laser vision correction after multifocal IOL implantation. J Refract Surg. 2008 Mar;24(3):274-9.
15. Woodard MA, Randlemann JB, Stulting RD. Dissatisfaction after multifocal intraocular lens implantation. J Cataract Refract Surg. 2009 Jun;35(6):992-7.
16. Chen YT, Tseng SH, Ma MC, Huang FC. Corneal epithelial damage during LASIK: a review of 1873 eyes. J Refract Surg. 2007 Nov;23(9): 916-23.
17. Shah VC, Russo C, Cannon R, et al. Incidence of Nd:YAG capsulotomy after implantation of AcrySof multifocal and monofocal intraocular lenses: a case controlled study. J Refract Surg. 2010 Aug;26(8):565-8.
18. Biber JM, Sandoval HP, Trivedi RH, et al. Comparison of the incidence and visual significance of posterior capsule opacification between multifocal spherical, monofocal spherical, and monofocal aspheric intraocular lenses. J Cataract Refract Surg. 2009 Jul;35(7):1234-8.
19. Soda M. Yaguchi S. Effect of decentration on the optical performance in multifocal intraocular lenses. Ophthalmogica. 2012;227(4):197-204.


