 |
The biggest risk factor for discontinuing contact lens wear is discomfort.1,2 Certainly, an underlying dry eye can decrease lens comfort. But contact lens–induced dry eye, or CLIDE, gives name to the individual who has no symptoms of dry eye without contact lenses but is symptomatic during contact lens wear.3 Although CLIDE is not traditionally associated with primary dry eye, contact lens discomfort may be an early symptom of a compromised tear film. Let’s discuss why this occurs and how to promote healthier, more comfortable contact lens wear.
Three Steps for Success
Here are a few strategies that have worked well in our practice to help optimize the lens wearing experience:
(1) Identify underlying risk factors. Although it is relatively easy to identify obvious eyelid margin diseases such as anterior blepharitis, lid margin irregularities or posterior blepharitis, other clinical entities are much less obvious.
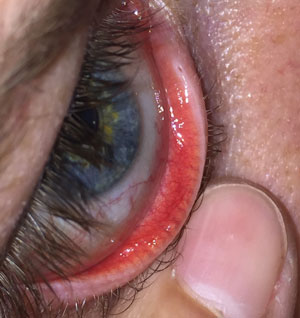 |
| Fig. 1. Gross observation of the meibomian glands on the lower lid. |
Consider floppy eyelid syndrome. The lid tarsus is often irregular, causing eyelids to flip easily. It is associated with sleep apnea, which should be discussed with the patient, along with a number of other local symptoms.4 Because of the loose lid apposition, the lids may inadvertently open and possibly evert, often in the evening, causing hyperemia and discomfort.5 Contact lens wear can be difficult for these individuals.
Another increasingly prevalent condition is non-obvious meibomian gland dysfunction (MGD). Through a standard exam the lid margin will typically appear normal, but dysfunction can be uncovered in a number of ways.6 The simplest test is to provide pressure to the upper and lower lid margin and assess the meibum expressed. Thickened lipids or lack of secretions indicate production abnormalities. The meibomian gland evaluator (TearScience) is a specialized instrument that applies a standard force to the lid margin, allowing an evaluation of the quality of meibum expressed.
We can also perform a gross inspection of the glands by having a patient look up and then pulling their lower lids down (Figure 1).
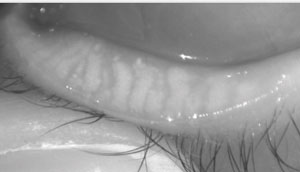
At the slit lamp, lid transillumination can also help us visualize the glands. With the slit beam turned off (a handheld transilluminator provides the only light source), have the patient look up, then place the transilluminator on the lower eyelid and slightly turn the lid down so that the palpebral conjunctiva is visible (Figure 2). Higher-level diagnostic imaging is also available to help better image the structure of the glands (Figure 3).
 |
| Fig. 2. Transillumination of the palpebral conjunctiva. |
(2) Educate patients. Making sure patients understand their condition is just as critical as identifying potential deficiencies. One of the most powerful educational tools is high-quality imaging, which provides patients a better perspective and actual visualization of their condition. Educating our patients is the first step to ensuring they comply with treatment.
(3) Help maintain, or regain, health. Following identification and education, we must treat the underlying condition. For individuals with floppy eyelid syndrome, for example, it is paramount to decrease inflammation and ensure the ocular surface is protected in the evening. This may include an ointment or the use of a Lacrisert (hydroxypropyl cellulose ophthalmic insert, Bausch + Lomb). Additionally, the patient may benefit from eye shields or taping their eyes shut in the evening. In severe instances, patients may also require eyelid surgery to re-establish normalcy to the lid/globe interaction.7
Chemical vs. Physical
While there are many approaches to non-obvious MGD treatment, we believe there are two global strategies: chemical and physical improvement of meibum production.
Chemical. Topical cyclosporine can promote healthier meibum production, and research shows the newly approved Xiidra (lifitegrast, Shire) improves symptoms of dry eye and may have a role in non-obvious MGD treatment as well.8,9 Topical azithromycin is another option for improving meibum production.10,11
 |
| Fig. 3. Meibography provides greater detail on meibomian gland status than clinical examination alone. Image: Dave Kading, OD. |
Essential fatty acids (omega-3s and omega-6s) have also been shown to improve meibum secretion.12,13 Additionally, oral doxycycline and oral azithromycin have proven effective in improving meibum production; although typically used with obvious forms of MGD, they may have a role here as well.13
Physical. Clinicians have come up with a number of ways to physically soften and evacuate stagnant meibum to allow healthier secretions. Traditionally, warm compresses once or twice a day were recommended. Although this can be done with warm, moist washcloths, there are logistical challenges to keeping the washcloths at the appropriate temperature for the intended time period. Many practitioners now recommend commercially available heating pads for at-home treatment.
The Lipiflow (TearScience) in-office treatment applies heat to the palpebral conjunctiva while simultaneously applying pressure through an inflatable air bladder on the anterior surface of the eyelid.14 One study shows a single treatment improved both signs and symptoms in individuals with MGD over 12 months.15 MiBoFlo Thermoflo (Mibo Medical) and the MGD 3000 (Ophthalmic Concepts) also heat the eyelid while gently massaging the lids.16,17
Seeing the Unseen
We challenge you to look for non-obvious clinical conditions in your contact lens wearers. If you discover them, educate patients and provide your best clinical judgment on the appropriate treatment. Your patients will thank you for taking the appropriate steps to improve their wearing experience and provide more comfortable lens wear.
Look for Signs Early For comparison, we would never wait to treat glaucoma patients until they become symptomatic. Glaucomatous damage is considered permanent, irreversible vision loss, so we seem to take it more seriously than dry eye, which improves wth treatment. However, this isn’t necessarily the right perspective. We now know there are early signs of damage or decreased functionality within the eyelid well before we see the consequences manifest on the ocular surface. It is critical to become hyper-observant of the lid to ensure appropriate care and maintenance of the lid margin, ultimately providing a higher quality tear film to help support lens wear. |
1. Rueff EM, Varghese RJ, Brack TM, et al. A survey of presbyopic contact lens wearers in a university setting. Optom Vis Sci. 2016;93(8):848-54.
2. Nichols JJ, Jones L, Nelson JD, et al., members of the TFOS International Workshop on Contact Lens Discomfort. The TFOS international workshop on contact lens discomfort: introduction. Invest Ophthalmol Vis Sci. 2013;54(11):TFOS1-6.
3. Fonn D. Targeting contact lens induced dryness and discomfort: what properties will make lenses more comfortable. Optom Vis Sci. 2007;84(4):279-85.
4. Skorin L Jr, Knutson R. Ophthalmic diseases in patients with obstructive sleep apnea. J Am Osteopath Assoc. 2016;116(8):522-9.
5. Mastrota KM. Impact of floppy eyelid syndrome in ocular surface and dry eye disease. Optom Vis Sci. 2008;85(9):814-6.
6. Blackie CA, Korb DR, Knop E, et al. Nonobvious obstructive meibomian gland dysfunction. Cornea. 2010;29(12):1333-45.
7. Pham TT, Perry JD. Floppy eyelid syndrome. Curr Opin Ophthalmol. 2007;18(5):430-3.
8. Prabhasawat P, Tesavibul N, Mahawong W. A randomized double-masked study of 0.05% cyclosporine ophthalmic emulsion in the treatment of meibomian gland dysfunction. Cornea. 2012;31(12):1386-93.
9. Holland EJ, Whitley WO, Sall K, et al. Lifitegrast clinical efficacy for treatment of signs and symptoms of dry eye disease across three randomized controlled trials. Curr Med Res Opin. 2016 Jul 22:1-7. [Epub ahead of print].
10. Foulks GN, Borchman D, Yappert M, et al. Topical azithromycin therapy for meibomian gland dysfunction: clinical response and lipid alterations. Cornea. 2010;29(7):781-8.
11. Liu Y, Kam WR, Ding J, Sullivan DA. One man’s poison is another man’s meat: using azithromycin-induced phospholipidosis to promote ocular surface health. Toxicology. 2014 Jun 5;320:1-5.
12. Liu Y, Kam WR, Sullivan DA. Influence of omega 3 and 6 fatty acids on human meibomian gland epithelial cells. Cornea. 2016;35(8):1122-6.
13. Qiao J, Yan X. Emerging treatment options for meibomian gland dysfunction. Clin Ophthalmol. 2013;7:1797-803.
14. Zhao Y, Veerappan A, Yeo S, et al. Clinical trial of thermal pulsation (Lipiflow) in meibomian gland dysfunction with preteatment meibography. Eye Contact Lens. 2016 Jan 27. [Epub ahead of print].
15. Blackie CA, Coleman CA, Holland EJ. The sustained effect (12 months) of a single-dose vectored thermal pulsation procedure for meibomian gland dysfunction and evaporative dry eye. Clin Ophthalmol. 2016 Jul 26;10:1385-96.
16. Mibo Medical Group. MiBoFlo ThermoFlo Management of Dry Eye. Available at http://mibomedicalgroup.com.
17. Ophthalmic Concepts. MGD 3000. Available at www.ophthalmicconcepts.com.


