
 Patients often report having been told they can’t wear contact lenses because of their astigmatism. With advancements in contact lens technology, however, this is no longer the case. Major soft lens manufacturers and custom soft lens laboratories now offer extended parameter ranges, allowing even the most highly astigmatic patients to fall within a correctable range.
Patients often report having been told they can’t wear contact lenses because of their astigmatism. With advancements in contact lens technology, however, this is no longer the case. Major soft lens manufacturers and custom soft lens laboratories now offer extended parameter ranges, allowing even the most highly astigmatic patients to fall within a correctable range. Despite advances in soft lens technology, however, the gold standard for quality of vision is still a gas permeable (GP) lens. Research shows GP lenses provide superior vision over their soft toric lens counterparts—including for patients with moderate to high astigmatism of 2.50D or greater.1
Although fitting GP lenses for astigmatism may seem intimidating, it’s essential knowledge for contact lens practitioners.
When to Use a Toric GP
The normal astigmatic cornea has two principal meridians 90 degrees apart, each with a different curvature and resultant refractive power. In combination with the tear layer underneath, a GP lens provides a spherical refracting surface to correct the astigmatism. To provide optimal comfort and vision, a GP lens should center well over the visual axis and align closely to the corneal shape.
Typically, you can successfully fit a spherical GP lens on a cornea with 2.0D or less of toricity. Before placing a spherical GP lens on the eye, you should calculate residual internal astigmatism, which originates from the posterior cornea and/or crystalline lens. The calculated residual astigmatism (CRA) is the difference between the total refractive astigmatism at the corneal plane and the anterior corneal astigmatism measured by keratometry. You can find actual residual astigmatism (ARA) by subjective spherocylindrical overrefraction. The ARA is typically less than the CRA, and simple math will save chair time and frustration, as 0.75D or more of ARA can result in decreased vision.2
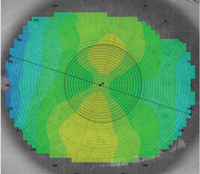 |
| This 3.0D with the rule cornea is a great candidate for a GP lens with back surface toricity. |
In this situation, if a GP lens is still indicated or preferred by the patient over a soft toric lens, you can fit a front surface toric (FST) GP lens. FST GP lenses apply the astigmatic power on the front surface, using prism ballasting and truncation to stabilize rotation. Similar to soft toric lenses, FST GPs may require rotational compensation using the left add, right subtract (LARS) principle.
As the corneal astigmatism increases, you should pay greater attention to the alignment of the GP lens to the corneal curvature. Placing a GP lens with a spherical back surface on a highly astigmatic cornea will create a dumbbell shaped sodium fluorescein pattern with apical bearing along the flat meridian, as well as pooling and edge lift along the steep meridian. This misalignment can cause several complications, including lens rocking or flexure; decentration; corneal molding and distortion; and corneal desiccation from excessive edge lift.
Although there is debate among practitioners, 2.50D or more of corneal astigmatism is a commonly accepted threshold for using back surface toricity.3 By using two base curves (BC), one for each principal meridian, back surface toricity provides a better lens-to-cornea fit. While several methods to determine BCs exist, the Mandell-Moore guide is a popular and efficient method. Using this fit factor, the BC is 0.25D flatter than the flat meridian and 0.50D to 0.75D flatter than the steep meridian, depending on the amount of corneal astigmatism. The lens power on each meridian is then determined, using the SAM-FAP principle to account for the tear lens power.
| The GPLI Toric Calculator |
| The GPLI Toric Calculator, available at www.gpli.info/lens-calculator, can help you select the correct lens parameters and either an SPE or CPE design. |
| Example 1: SPE Spectacle Rx: -1.00-3.25x180 Ks: 42.00/45.00 |
 |
| BC: 42.00/44.25 BVP: -1.00/-3.25 ΔBC (2.25 D) = ΔBVP (2.25 D) |
| Example 2: CPE Spectacle Rx: +1.00-4.50x180 Ks: 42.00/45.50 |
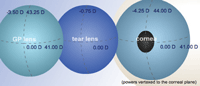 |
| BC: 42.00/44.75 BVP: +1.00/-2.50 ΔBC (2.75 D) ≠ ΔBVP (3.50 D) |
| Example 3: BST Spectacle Rx: plano-4.50x180 Ks: 41.00/44.00 |
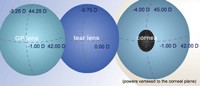 |
| BC: 41.00/43.25 BVP: 0.00/-3.50 ΔBC (2.25 D) x 1.5 ≈ Δ BVP (3.50 D) |
Bitoric Lenses
Because of differences in the refractive index of the contact lens and the tear lens, a GP lens with back surface toricity will induce astigmatism of approximately half the magnitude of the back surface toricity. In most cases, to correct this induced astigmatism, you can add additional astigmatic power to the front surface of the lens, making the lens bitoric.
Bitoric lenses are classified into two designs: spherical power effect (SPE) and cylindrical power effect (CPE). When adding astigmatic power to the front surface of the lens, you must take rotation of the lens into consideration. SPE lenses correct astigmatism similar to a spherical lens, despite having bitoric curves. Thus, the lens power is equivalent to a spherical lens and can rotate freely on the eye without impacting vision. CPE lenses must be rotationally stable to avoid inducing further astigmatism.
To determine the bitoric design, you should compare both the dioptric BC difference and the back vertex power difference between the two principle meridians. If the dioptric differences between meridians are equal for both BC and back vertex power, the bitoric is an SPE design. When the dioptric differences are unequal, the lens is a CPE design—typically occurring when refractive astigmatism is unequal to corneal astigmatism.
If the back vertex power is 1.5 times the back surface toricity, the induced astigmatism effectively cancels out the residual astigmatism. In these cases, the front surface of the GP can be made spherical, resulting in a back surface toric only lens. While this concept may be confusing, most laboratories will determine the necessity for you.
Toric GP Fitting Made Easy
Before the days of empirical ordering, diagnostic fitting was performed with standard SPE fitting sets and overrefraction calculations. Now, you can design a toric GP lens with a high degree of accuracy using only keratometry readings and manifest refraction.1 You can provide this data directly to your GP lab of choice; however, if you prefer to calculate the math yourself, the GP Lens Institute (www.gpli.info) has several guides available, including a Mandell-Moore worksheet. Additionally, there is a GP toric calculator, which provides suggested lens parameters and indicates whether the lens is an SPE or CPE design. These resources can help improve your toric fitting confidence.
1. Michaud L, Barriault C, Dionne A, Karwatsky P. Empirical fitting of soft or rigid gas-permeable contact lenses for the correction of moderate to severe refractive astigmatism: A comparative study. Optometry. 2009 Jul;80:375-83.
2. Sarver MD. A study of residual astigmatism. Am J Optom. 1969;46(8):578-82.
3. Bennett ES, Layfield KA, Lam D, Henry VA. Correction of astigmatism. In: Bennett ES, Henry VA, eds. Clinical Manual of Contact Lenses. 4th Ed. Philadelphia: Lippincott, Williams & Wilkins; 2014:344-94.


