Unlike many diseases, the challenges of keratoconus do not end when your treatment begins. While a recognized and legitimate medical condition and medical diagnosis, keratoconus poses a unique challenge in the insurance reimbursement arena.
Think about it this way: Medical carriers cover medical conditions; therefore, the professional service aspect of managing the keratoconic patient may be covered by that entity. However, the treatment aspect of keratoconus involves contact lenses, which—despite being an approved medical device by the FDA—are generally not covered by the patient’s medical insurance. If the patient doesn’t have a specific refractive insurance plan with generous material benefits, the largest portion of significant cost is not covered.
This poses considerable challenges for the average optometrist who is diagnosing and treating keratoconus patients. Why? The dilemma here is mostly psychological. Optometrists typically don’t want the patient to have to pay for anything out-of-pocket and tend to want to treat things that have some insurance coverage.
That being said, the smartest practitioners (the ones who actually follow the rules that are in place) have figured out that keratoconus is analogous to orthodontics—patients have a condition that requires treatment and may have limited or no coverage for its treatment and the patient is required to pay the full dollar amount out-of-pocket. This means no reductions, no insurance maximum allowances and no write-offs. Admittedly, this isn’t easy to do, since most practitioners have a hard time reconciling profitability for their practice with the expense on the patient. But remember: if they don’t pay you, they’ll pay someone else.
Simply put, although we clearly recognize keratoconus as a medical condition, many medical carriers and refractive carriers don’t recognize it as a covered service or condition. (One notable exception is VSP, who actually has, in my opinion, a fairly generous keratoconus benefit.)
This brings up a critical concept: You cannot create coverage for a patient where no coverage exists. If the patient doesn’t have coverage (benefits) for keratoconus treatment, they simply will have to pay out-of-pocket; while unfortunate for the patient, this translates to greater profitability for your practice.
New Codes, New Coverage?
Keratoconus patients often present optometrists with several challenges. First, it can be very difficult to provide clear, comfortable vision without investing considerable chair time. The next greatest hurdle is receiving proper reimbursement for that time you invested.
Let’s look at how to navigate these obstacles together to help you offer the highest level of clinical services to your patients while making sure that you are 100% compliant with the current rules.
Initial Exam and Diagnosis
The diagnosis of keratoconus is typically suspected or made during your general examination, and then confirmed by corneal topography and/or pachymetry. Medical carriers vary considerably in their reimbursement policies for topography reimbursement. Unfortunately, many won’t pay for the procedure, regardless of your appeals. It is important that you know your carrier’s policies and use an ABN form appropriately to ensure that you are still getting paid for this service (more on that later).
 Once you confirm the diagnosis and counsel the patient, finalize your decision to fit the patient in contact lenses. Make sure to record this as an order in your patient’s medical records. This compliance step is critical to establishing the medical necessity for the subsequent fitting and management office visits.
Once you confirm the diagnosis and counsel the patient, finalize your decision to fit the patient in contact lenses. Make sure to record this as an order in your patient’s medical records. This compliance step is critical to establishing the medical necessity for the subsequent fitting and management office visits.
The initial visit—a general exam—is generally billed either to the patient or the refractive carrier. Keep in mind that it is the chief complaint that drives the responsible party, not the ultimate diagnosis. Also remember that, for patients who have refractive as well as medical benefits, we have to adhere to the coordination of benefits requirements specific to the individual policy. This means that often the refractive carrier will be covering the 920X4 and 92015. Unfortunately, this is the first step where many offices fail to bill correctly and try to improperly bill the medical carrier because of the keratoconus diagnosis.
The First Fitting
Despite the efforts of many, the code for bandage lens fitting and supply (92070) was a poor choice for keratoconus, and in fact was eliminated by the CPT in January 2012. It is no longer a code that is recognized by either medical or refractive carriers.
Instead, a new CPT code developed in January 2012 was specifically designed for the fitting of a keratoconus patient. Note: The CPT is very specific about how a practitioner is to use the code and how to bill for the initial fitting and all subsequent office visits. This code is different than the CPT code used for traditional non-keratoconic fits.
• CPT Code 92310: For a traditional contact lens fit, this code correlates with a “prescription of optical and physical characteristics of and fitting of a contact lens, with medical supervision of adaptation; corneal lens, both eyes, except for aphakia.” This code encompasses all services that are provided until you write a contact lens prescription. It is charged at each visit during which a new lens is placed on a patient’s eye or a fit is altered, but does not include contact lens follow-up care after the lenses have been dispensed.
Keep in mind that the modifier (-52) should be used if fitting only one eye (see “-52 Reduced Services” above). This is a change from 2011.
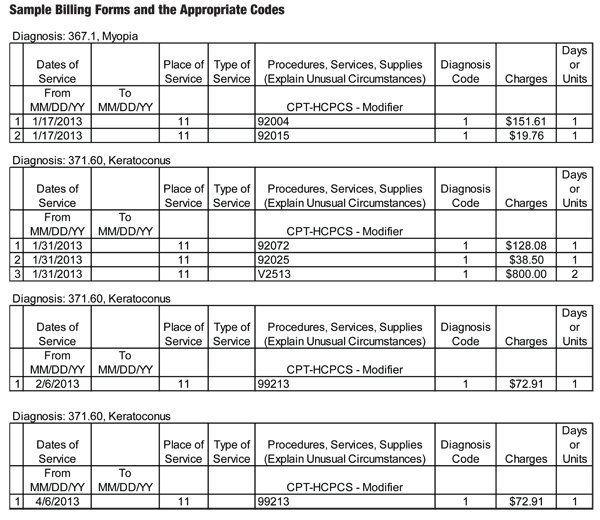
• CPT Code 92072: This code is used for the fitting of a contact lens for the management of keratoconus. Using code 92072 covers the initial fitting examination for professional services only. In mid-2012, this code was changed from a unilateral code to a bilateral code, so you get paid once for fitting both eyes.
All subsequent office visits are to be billed using the appropriate level evaluation and management codes 9921X or the appropriate level ophthalmic codes 9201X. Please report materials (lenses) in addition to this code using either 99070 or the appropriate HCPCS Level II material code (such as V2513 or V2531) for gas-permeable extended wear lens.
Each and every visit should be properly documented in the medical record with your patient’s reason for visit and subsequent treatment plan. Always remember that the record should reflect your thoughts and impressions as well as physical findings. Again, if the patient doesn’t have coverage for the materials, they will have to pay out-of-pocket for them.
Refitting and Monitoring
CPT contact lens services state: “The fitting of contact lens includes instruction and training of the wearer and incidental revision of the lens during the training period.” If complications arise, the most appropriate way to bill for office visits is using the established patient ophthalmologic (9201X) or evaluation and management (9921X) codes.
When billing the medical carrier for these office visits, keep in mind the need to use the appropriate diagnosis for the corneal condition you are monitoring. Note: You’re not performing a contact lens follow-up; the reason for the office visit is to monitor the corneal condition, not the lens!
To summarize, never consider a fitting fee to be a global, year-long obligation to provide unlimited service at no charge. If you refit a patient, it is not just an “incidental revision of the contact lens;” according to the CPT, you should refit the patient using a 9201X or 9921X code, along with the appropriate materials V-code for lens supply.
And a final word of advice: Don’t make the mistake of discounting your services if the patient has to pay directly. Bill all parties equally and without bias.
Dr. Rumpakis is President of PRMI, a healthcare-based consulting firm. He is a nationally known expert in the area of medical coding and compliance and is the founder of ReimbursementPLUS.com, an industry leading cloud-based CPT Data & Information Service. He can be reached at [email protected].


