 Astigmatism is something we all troubleshoot on a daily basis. Most of the time, we are working with regular astigmatism produced by the shape of the cornea or the lens, but there is also irregular astigmatism caused by corneal dystrophies, degenerations and scarring. In this article, we are tackling both types of astigmatism by utilizing a customized scleral gas-permeable contact lens.
Astigmatism is something we all troubleshoot on a daily basis. Most of the time, we are working with regular astigmatism produced by the shape of the cornea or the lens, but there is also irregular astigmatism caused by corneal dystrophies, degenerations and scarring. In this article, we are tackling both types of astigmatism by utilizing a customized scleral gas-permeable contact lens.
TH, a 51-year-old white male, visited our office for a corneal evaluation and possible contact lens fitting. He was seeking a second opinion on the progression and treatment of his keratoconus, which was previously diagnosed 10 years ago. Even though he was a well-adapted GP contact lens wearer, he still struggled to wear his corneal sized contact lenses for a full day. He battled with fluctuating vision and lens discomfort, and noted he has lost many lenses in the past due to an unstable fit.
Visual acuities were 20/50 O.D. and 20/40 O.S. through his current contact lenses. Subjective refraction yielded -4.75-2.50x075 O.D. and -4.00-4.25x100 O.S. There was no corneal scarring noted on slit lamp examination. Topographies were consistent with pellucid marginal degeneration and simulated keratometry readings were 43.87x41.12 @ 064° O.D. and 45.37x42.12D @ 104° O.S.
Scleral Lens for PMD
The corneal changes that occur with pellucid marginal degeneration (PMD) can make for a challenging contact lens fitting. Soft toric contact lenses are unstable and typically don’t provide adequate visual acuity. Corneal or intralimbal sized GP contact lenses often rest at a low position due to the inferior corneal steepening, especially in moderate or severe PMD. The most successful contact lens fittings take the corneal irregularity out of the fitting process and utilize a scleral contact lens design to better align with the regular curvature of the sclera.
We began the scleral contact lens fitting process after discussing their benefits, and how his problems associated with contact lens wear related to his corneal condition. The initial diagnostic lenses were Jupiter GP scleral contact lenses, 18.2mm in overall diameter. The selected base curves were 48.00D O.D. and 49.00D O.S.
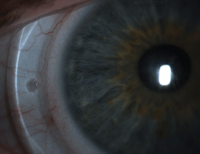
Engraved markers at the three and nine o’clock positions aid in evaluation of rotation and rotational stability.
There was adequate corneal and limbal clearance, with only mild conjunctival blanching. An over-refraction yielded about a diopter of astigmatism in each eye, with best corrected acuities of 20/20 O.D. and 20/25 O.S. New lenses were ordered with flatter peripheral curves and an increased center thickness to decrease lens flexure and eliminate over-refractive astigmatism.
At his dispensing visit, the new Jupiter scleral contact lenses were evaluated. Visual acuity was 20/20 O.D. and 20/30 O.S. The contact lens fit was satisfactory and an over-refraction yielded nearly a plano result O.D., but yet again, a diopter of astigmatism in the left eye at a similar axis to the over-refraction of the initial trial lens and his manifest refraction. A new scleral lens was ordered for TH in a toric front surface design to correct the over-refractive astigmatism.
Scleral Lenses for Astigmatism
When working with scleral contact lenses, a spherical over-refraction is usually all that is needed to correct the patient’s vision. But, when a patient’s acuity is less than satisfactory, consider a sphero-cylindrical over-refraction to maximize vision potential. Over-refractive astigmatism with a scleral contact lens results from a couple scenarios. The most common scenario is lens flexure, with is easily corrected by increasing the lens’ center thickness by 0.1mm or 0.2mm. You can verify lens flexure by measuring the curvature of the lens surface by topography or an over-keratometry reading while the patient is wearing the lens. The lens is flexing if the difference in keratometry readings correspond to the amount of astigmatism in the over refraction. If the keratometry readings are spherical, there is likely lenticular astigmatism, and utilizing a front-surface toric lens design can improve visual acuity and quality.
TH returned to the office wearing his new left lens, and was still unhappy with his vision. His visual acuity was 20/50 with a wearing time of less than one hour. Evaluation revealed that the toric lens was positioned obliquely, and once the lens was properly rotated on the eye his visual acuity improved to 20/20 with minimal over-refraction. The lens rotation remained stable for the remainder of the visit. TH was then instructed on how to apply the lens with the toric markers properly positioned to allow the lens to settle quickly at the desired orientation.
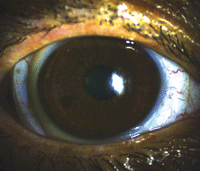
This front surface toric lens is slightly rotated immediately after application.
Front Surface Toric Scleral Lenses
Front surface toric scleral contact lenses have engraved toricity markers at the three and nine o’clock positions. The lenses have a double slab-off peripheral curve system to create a rotationally stable contact lens. Most patients can easily identify the lens markings prior to applying the lens, which allows for near perfect vision immediately after application. If the patient cannot identify the lens markings due to poor uncorrected acuity or presbyopia, they are taught to apply the lens normally and then use a clean finger to spin the lens on the eye until their vision is clear and crisp.
At a follow up visit, TH was very pleased with his contact lenses. He raved about the lens comfort and stability, and noted that his vision was better than ever.
This case is just another example of ways to further customize a specialty scleral contact lens for the visual needs of our unique patients.


