 |
Ocular surface disease. Meibomian gland dysfunction. Blepharitis. Every eye care meeting is teeming with lectures on these topics, and rightly so. Although practitioners have always seen a multitude of patients with complaints of dryness, irritation and redness, it is only recently that diagnostic tools and treatments have improved enough to better pinpoint the exact problem and treat each individual patient appropriately and more effectively than ever before.
But there’s one more word that needs to be incorporated into our daily lexicon: Demodex. While we may not wish to embrace the notion that infestation of this intradermal parasitic mite is the cause of a host of eyelid problems, we cannot ignore the facts.
Consider this: in a study by Hyun Koo, MD and colleagues, Demodex were found in 84% of patients with ocular discomfort (i.e., dryness, pruritus, ocular pain, or visual disturbance).1 Prevalence was also found to increase with age: Demodex was identified in 84% of the population at age 60 and 100% of the population over the age of 70.2
These are staggering statistics for a condition that is routinely overlooked. Many of us have patients in our practice who we are doggedly treating for blepharitis, with little to marginal improvement. In cases like this, we need to consider that Demodex could be the cause when the problem is refractory to the standard therapies of artificial tears, warm compresses or prescription topical or oral antibiotic or steroid formulations. First, however, we need to know how to identify a Demodex-laden lid and then how to eradicate the problem.
|
|
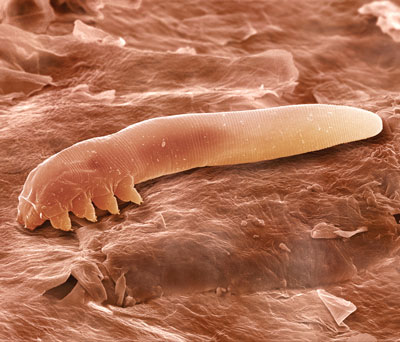
| Fig. 1. Demodex, pervasive on lids and lashes, can clog the meibomian glands. ©PS Micrographs |
A Mite-y Challenge
A classic presentation of Demodex blepharitis appears as cylindrical, waxy collarettes at the base of the eyelashes, thought to be an accumulation of Demodex folliculorum excreta, epithelial hyperplasia and reactive hyperkeratinization.3-4 The mites consume epithelial cells at the hair follicle, causing lash distention.
Infestation is caused primarily by Demodex brevis, which reside deep in the meibomian glands, leading to blockage and lipid tear film insufficiency, and sometimes recurrent and refractory chalazia.5,6 Dying mites themselves may trigger a cascade of inflammatory responses involving the lid margin, conjunctiva and cornea that can be visually devastating.4
Often, the mites are not easily visible at the slit lamp. Traditional examination involves the epilation of four non-adjacent eyelashes that are evaluated under a microscope. However, a newer method has recently been described in which, with gentle tension, the eyelash is rotated manually with forceps scraping around the inner perimeter of the eyelash follicle to dislodge nonvisible mites that may reside deeper within the lash follicle.7,8 This rotational maneuver may help isolate Demodex mites in follicles whose lashes may not display the characteristic tubular base cuffing. However, additional research is needed to determine the efficacy of this technique.
Tea tree oil has been previously shown to be effective in treating Demodex, though early treatments with the full-strength formulation proved irritating to some patients and required cumbersome in-office dilution. Ying-Ying Gao, MD and Jingo Liu, MD, among others, have demonstrated lid scrub with 50% strength tea tree oil and/or lid massage with 5% tea tree ointment and the use of tea tree oil shampoo to be effective in eradicating ocular Demodex. The treatments worked either by directly killing the mites or interrupting their life cycle by preventing mating, with marked subjective and objective improvement noted in the lid margin, conjunctiva and cornea.9,10
|
|
|
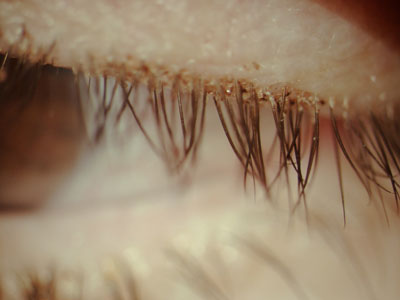
| Fig 2. Collarettes around the base of lashes is a predictable sign of Demodex. |
Cliradex (Bio-Tissue) is a pre-moistened lid, lash and facial towelette that contains the specific ingredient in tea tree oil, 4-terpineol, that has been shown to be the most efficacious in killing Demodex in vivo.11 The wipes are recommended for once daily use for six to eight weeks for mild to moderate symptoms, or twice daily use for six to eight weeks for moderate to severe symptoms.12 The new Cliradex Complete Advanced Lid Hygiene Kit also contains a stronger concentration of 4-terpineol for in-office application by a doctor or trained technician for more severe cases of Demodex, in addition to the wipes for at home use.
The FDA recently approved Advanced i-Lid Cleanser (NovaBay Pharmaceuticals), a liquid lid and lash cleanser formulated with 0.001% hypochlorous acid (called Neutrox), a broad-spectrum antimicrobial.13 While the product is indicated for use against organisms such as Staph. aureus and epidermidis, as well as methicillin-resistant Staph. aureus (MRSA), NovaBay says its independent studies suggest that cleansing may also help reduce Demodex-associated bacteria and minimize the inflammatory cascade caused by the bacterial exotoxins.14
Additional Demodex-fighting options include the BlephEx in-office exfoliation procedure from Rysurg, Ocusoft’s Lid Scrub Plus, over-the-counter cleansers from Ovanté, and other interventions.
As we increasingly encounter an aging population, we need to be fully cognizant of the possibility that many of these patients may have Demodex as a contributing factor in their eyelid and ocular surface dysfunction. Fortunately, we have simple and effective in-office and at home treatments to eradicate the problem.
1. Koo H, Kim TH, Kim TW et al. Ocular Surface Discomfort and Demodex: Effect of Tea Tree Oil Eyelid Scrub in Demodex Blepharitis. J Korean Med Sci 2012; 27: 1574-1579.
2. Post CF, Juhlin E. Demodex folliculorum and blepharitis. Arch Dermatol. 1963;88:298–302.
3. Gao YY, Di Pascuale MA, Li W, et al. High prevalence of Demodex in eyelashes with cylindrical dandruff. Invest Ophthalmol Vis Sci 2005;46:3089-94.
4. Bevins CL, Liu FT. Rosacea: skin innate immunity gone awry? Nat Med 2007;13:904–906.
5. Gao YY, Di Pascuale MA, Elizondo A, Tseng SC. Clinical treatment of ocular demodecosis by lid scrub with tea tree oil. Cornea 2007;26:136–143.
6. Koksal M, Kargi S, Taysi BN, Ugurbas SH. A rare agent of chalazion: demodectic mites. Can J Ophthalmol 2003;38:605–606.
7. Mastrota KM. Method to identify Demodex in the eyelash follicle without epilation. Optom Vis Sci. 2013 Jun;90(6):e172-4.
8. Por YM. Demodex blepharitis – Is it for real? www.youtube.com/watch?v=sgav_kZ_Hi4
9. Gao YY, Di Pascuale MA, Li W, Baradaran-Rafii A, et al. In vitro and in vivo killing of ocular Demodex by tea tree oil. Br J Ophthalmol 2005; 89: 1468-73.
10. Liu, J, Sheha H, Tseng S. Pathogenic role of Demodex mites in blepharitis. Curr Opin Allergy Clin Immunol. 2010 October; 10(5): 505–510.
11. Tighe S, Gao YY, Tseng SCG. Terpinen-4-ol is the most active ingredient of tea tree oil to kill demodex mites. Transl Vis Sci Technol. 2013 Nov;2(7):2.
12. www.biotissue.com/products/about-cliradex
13. Wang L, Bassiri M, Najafi R, et al. Hypochlorous acid as a potential wound care agent: part I. Stabilized hypochlorous acid: a component of the inorganic armamentarium of innate immunity. J Burns Wounds. 2007 Apr 11;6:e5.
14. http://novabay.com


