 When it comes to fitting irregular corneas, practitioners often choose scleral lenses. We want to recreate a new refractive surface through a rigid gas-permeable (GP) lens. As with more traditional, smaller-diameter GPs, the rigid surface of scleral lenses renormalizes the surface.
When it comes to fitting irregular corneas, practitioners often choose scleral lenses. We want to recreate a new refractive surface through a rigid gas-permeable (GP) lens. As with more traditional, smaller-diameter GPs, the rigid surface of scleral lenses renormalizes the surface.
But scleral lenses have two additional qualities. By vaulting over the cornea, scleral lenses are not dependent on lens-to-cornea interaction. And by bearing the weight on the surrounding conjunctiva and underlying sclera, large-diameter lenses do not move like traditional GP lenses. Thus, there is significantly less lens awareness.
Traditionally, we have considered scleral lenses for corneas with significant irregularities. But, can these lenses also benefit other patients with high visual demands?
Fitting the Astigmatic Patient
We generally tend to fit our astigmatic patients in toric soft lenses, even though this may be a suboptimal choice due to rotational stability issues. What if, instead, we considered using GP lenses? Depending on the level of corneal astigmatism and its relationship to refractive astigmatism, a patient may do well in a standard spherical, a back surface or a bitoric GP design. These designs correct the astigmatism that is dependent upon a tear layer between the posterior surface of the lens and corneal surface, as well as address toric surfaces that may be made in the lens.
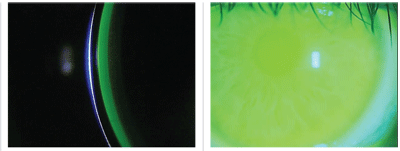
1. Central clearance that is equal to the thickness of the contact lens (left). 2. View of the lens showing fluorescein over the whole cornea (right).
A potential disadvantage to a traditional GP, however, is the initial additional lens awareness that a patient may experience relative to a soft toric lens. On the other hand, a scleral lens bears its weight on the conjunctiva and underlying sclera as opposed to the cornea. Because it rests on the conjunctiva, it does not move like a corneal GP lens and thus patients experience very little lens awareness while still benefitting from the optics of a GP.
Here, we will review the three major considerations when fitting scleral lenses so as to improve your chances for success.
1. Central corneal clearance. Because a scleral lens rests on the conjunctiva, an ideal fit will vault over the cornea without ever touching it. Although there has been no standard as to how much or how little clearance is required, many practitioners have adopted a clearance of 100µm to 300µm.1 Although the clearance can be measured with an anterior segment OCT, most practitioners will estimate the clearance using the corneal thickness as a reference.
Before the lens is placed on the eye, the bowl is filled with non-preserved saline. Fluorescein is then added to the bowl, usually via a strip, to help easily visualize the saline between the posterior surface of the lens and the front surface of the cornea. After the lens is placed on the eye, an optical section through the lens and cornea will reveal the amount of clearance the lens demonstrates.
Because you already know the thickness of the contact lens that you are fitting, you can approximate the clearance by estimating the thickness of the fluorescein as compared to the thickness of the lens (figure 1).
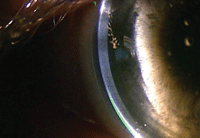
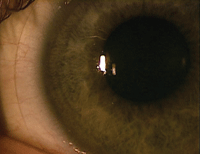
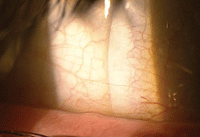
3. No fluorescein present in the limbal area between the cornea and scleral lens (left). 4. Ideal landing zone relationship (middle). 5. A steep landing zone causing conjunctival blanching inside the edge of the lens (right).
2. Limbal clearance. The guidelines for the amount of clearance in the limbal area are less specific. The most important point to remember is that the lens must clear the limbal region, which can be seen by visualizing that the fluorescein completely covers the cornea beneath the lens (figure 2). Additionally, viewing the clearance with an optical section should reveal fluorescein present between the posterior surface of the lens and the front surface of the cornea.
If no fluorescein is present, the lens is bearing on the limbus (figure 3). In this instance, the peripheral relationship of the lens will likely need to be steepened in order to prevent limbal bearing.
3. Landing zone. Ideally, the landing zone will rest tangentially on the conjunctival surface and will distribute the weight of the lens evenly throughout this area. This should cause no change in the architecture of the conjunctival vasculature (figure 4). If the landing zone is steeper or flatter than the surrounding scleral trajectory, there will be unintended pressure on the surrounding conjunctival tissue––potentially causing either vascular blanching or vascular engorgement (figure 5).
Understanding how scleral lenses can potentially deliver our astigmatic patients more stable vision can fill a void in the care we provide. In fact, it can help patients who may have otherwise discontinued contact lens wear to stay in their lenses and derail potential dropouts.
1. van der Worp E. A guide to scleral lens fitting [monograph online]. Scleral Lens Education Society. 2010. Available at: http://commons.pacificu.edu/mono/4/. Accessed February 2013.


